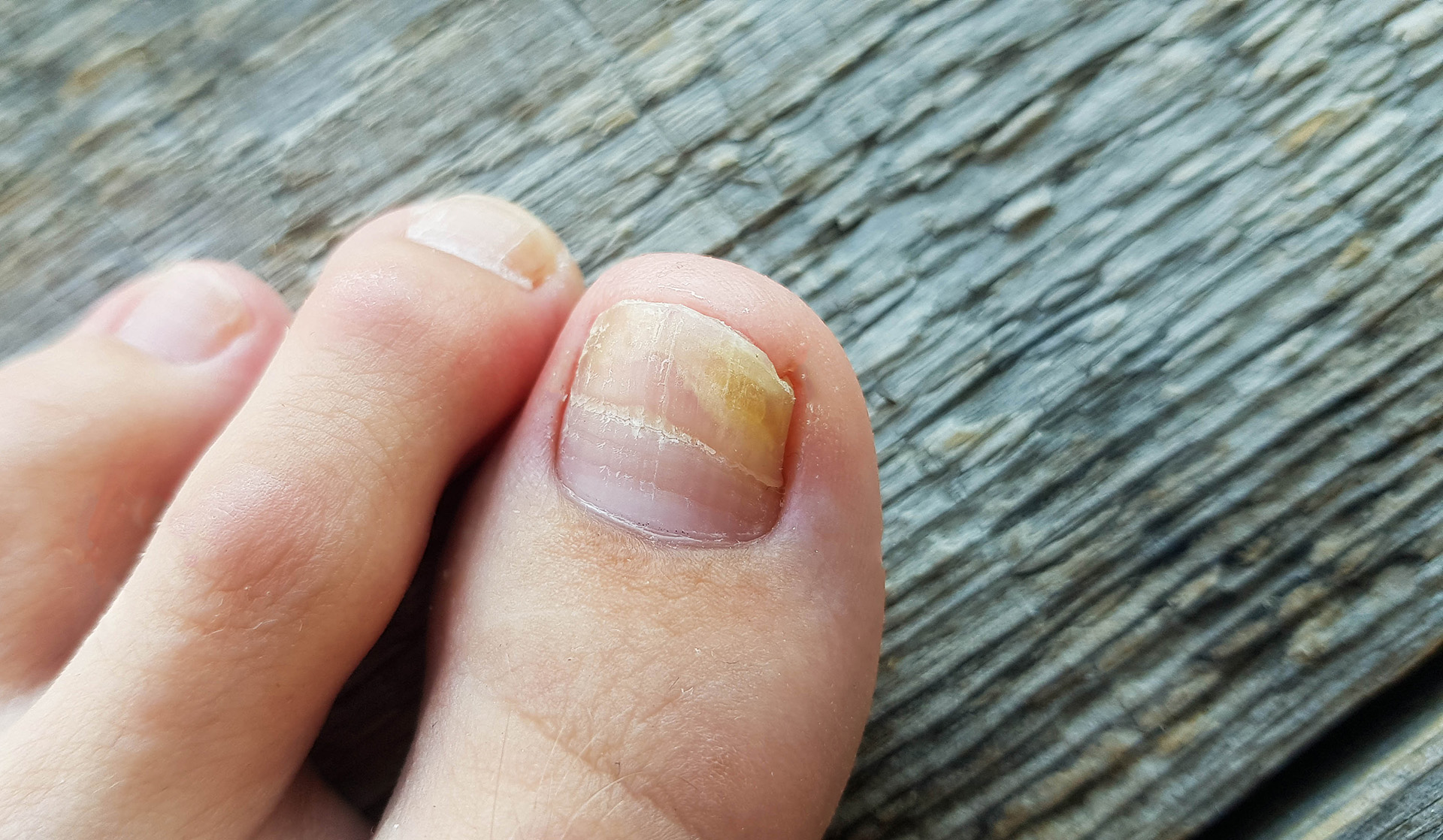
Fungal nails, or onychomycosis, can develop in both the toenails and fingernails. The problem occurs when fungi enter through small cracks in the nail or adjacent skin, resulting in visible changes such as discoloration or thickening. Fungal nail conditions do not usually pose severe health threats, but they may impact nail appearance and comfort. Here’s more information about this condition:
Understanding Fungal Functions
Fungi responsible for nail problems are microscopic organisms. Dermatophytes, the most frequent culprits, require keratin for growth; this is a protein found in nails, skin, and hair. Yeasts, such as Candida species, and certain non-dermatophyte molds also contribute to fungal nails. These fungi exist throughout the environment. When the area under the nail retains warmth, moisture, and darkness, it forms an environment favorable to fungal growth.
Contact with contaminated surfaces introduces fungi to the nails. Once established beneath the nail plate, the fungi begin to multiply and change the nail’s structure over time. Environmental conditions play a significant role in supporting this process.
Identifying Environmental Factors
Environments that are warm and moist are favorable for fungal survival. Walking barefoot in these areas increases the likelihood of fungi accessing toenails and surrounding skin. These public areas include:
- Swimming pools
- Gyms
- Locker rooms
- Showers
Daily habits can also contribute to the development of fungal nails. Consistently wearing the same shoes without allowing them to dry properly contributes to moisture retention. Wearing footwear constructed from non-breathable materials maintains a humid environment around the foot; this can lead to discomfort and other issues. Choosing socks that absorb sweat, rotating footwear, and allowing shoes to dry thoroughly between uses are all helpful habits for preventing foot problems.
Examining Health Factors
Individual health characteristics have a fundamental influence on vulnerability to fungal nails. A weakened immune system may allow fungi to develop with fewer obstacles, and age further influences risk. Nails naturally become drier and brittle with time, sometimes developing cracks or splits that provide entry for fungi. Poor blood circulation may hinder the body’s response to early fungal invasion. Minor injuries also create potential entry points for these organisms; this can result from trimming nails too closely, wearing tight shoes, or experiencing repeated trauma.
Practicing Nail Care
Good hygiene and thoughtful nail care are fundamental strategies for reducing the risk of fungal nail infections, and effective prevention doesn’t require complex measures. A consistent approach makes a substantial difference, such as:
- Keeping the nails clean, dry, and trimmed short.
- Wearing moisture-wicking socks and shoes that allow air circulation.
- Using protective footwear in shared, damp environments such as pools and locker rooms.
Regularly changing socks, particularly following exercise or sweating, limits moisture build-up. Clean, dry shoes that receive adequate time to air out between uses reduce favorable conditions for fungi. Individuals may also contemplate the use of antibacterial or antifungal powders if additional protection is deemed necessary.
Treat and Prevent Fungal Nails
Fungal nails develop through a combination of factors, including fungal presence, environmental exposure, personal habits, and underlying health issues. By identifying potential entry points for fungi and maintaining helpful daily routines, individuals can take meaningful steps to support nail health. If you develop this condition, consult a foot and ankle specialist for treatment using antifungal creams or oral medications. Contact a healthcare professional today for more information or to explore prevention strategies.